
Periodontal disease, also known as gum disease, is a common condition that affects the gums and supporting structures of the teeth. It is caused by bacteria present in dental plaque, which is a sticky film that forms on the teeth.
When plaque is not adequately removed through proper oral hygiene practices such as brushing and flossing, it can lead to inflammation of the gums, known as gingivitis.
Gingivitis is the early stage of periodontal disease and is characterized by red, swollen, and tender gums that may bleed easily, particularly during brushing or flossing. At this stage, the disease is still reversible with proper dental care and oral hygiene.
No, gingivitis is not a contagious disease. Gingivitis occurs when plaque bacteria build up on the teeth and gums which causes inflammation and bleeding of the gums.
Is periodontal disease contagious?
If left untreated, gingivitis can progress to periodontitis. Periodontitis is a more severe form of gum disease that involves the destruction of the bone and tissues that support the teeth. The bacteria in plaque release toxins that irritate the gums, causing an inflammatory response.
This leads to the formation of pockets between the gums and teeth, which further traps plaque and bacteria. As the disease progresses, the pockets deepen, and the bacteria can destroy the bone and connective tissues, resulting in tooth loss.
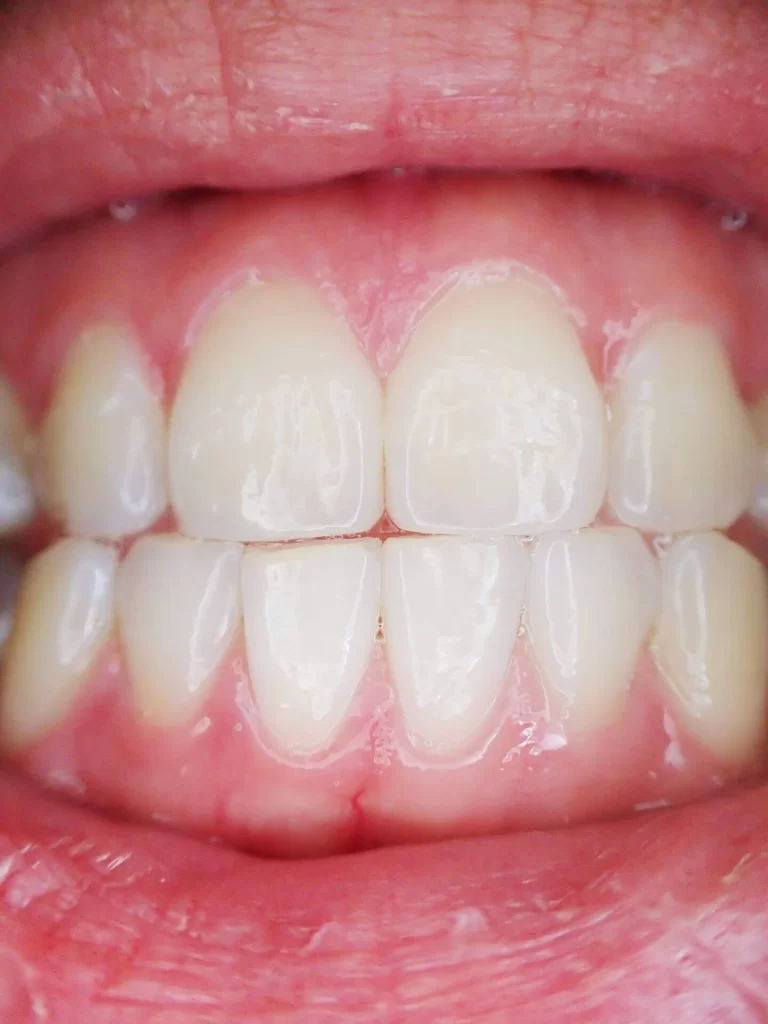
What are the causes for periodontal disease?
Periodontal disease is influenced by various factors, including poor oral hygiene, smoking, hormonal changes (such as during pregnancy or menopause), certain medications, genetic predisposition, and systemic diseases like diabetes. Periodontal disease can affect individuals of all ages, not just older adults.
It could be prevented by maintaining good oral hygiene practices, such as regular brushing and flossing, along with routine dental check-ups. It is also important to avoid tobacco use, maintain a healthy diet, and manage systemic conditions that may contribute to gum disease.
Is it a Contagious Disease?
Periodontal disease is not considered a contagious disease in the traditional sense. It is not typically transmitted through casual contact or airborne particles like the common cold or flu. However, the bacteria that contribute to gum disease can be transferred from person to person through certain activities that involve close contact or the sharing of oral hygiene items.
For example, if someone with active gum disease has bleeding gums and shares a toothbrush, dental floss, or other oral hygiene tools with another person, there is a possibility that the bacteria present in their mouth could be passed on to the other person. Similarly, activities such as kissing or intimate contact that involve the exchange of saliva can also potentially transmit the bacteria associated with gum disease.
It is always advisable to maintain good oral hygiene and avoid sharing oral hygiene items to minimize the potential spread of bacteria associated with gum disease.
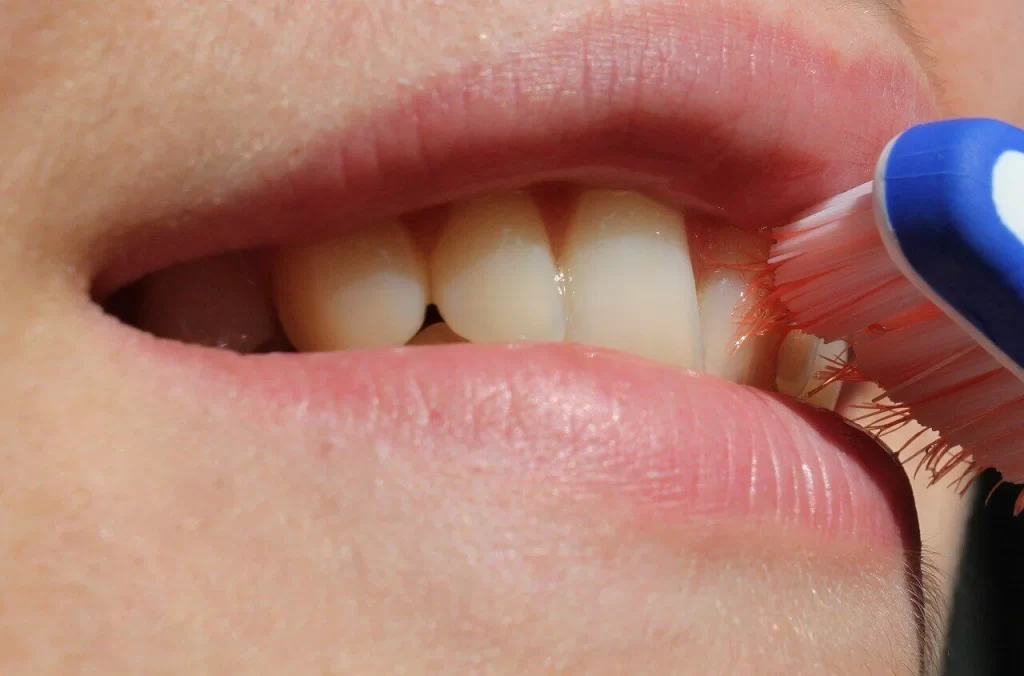
What Are the Symptoms of Periodontal Disease?
The symptoms of periodontal disease can vary depending on the stage and severity of the condition. The two main stages of gum disease are gingivitis and periodontitis, and their symptoms include:
Gingivitis
- Red, swollen, or inflamed gums
- Tender or sensitive gums
- Gums that easily bleed, especially during brushing or flossing
- Persistent bad breath
- Receding gums (gums appearing to pull away from the teeth)
- Formation of pockets between the gums and teeth
- Changes in the bite or the way the teeth fit together
Periodontitis (in addition to the symptoms of gingivitis):
- Chronic bad breath or a persistent unpleasant taste in the mouth
- Deepening of the pockets between the gums and teeth
- Loose or shifting teeth
- Changes in the way the teeth fit together or a noticeable change in the bite
- Gum recession leading to tooth sensitivity
- Formation of abscesses or pus between the teeth and gums
- Visible changes in the gums, such as gum recession or changes in color (gums appearing redder or purplish)
If you notice any of the above symptoms or have concerns about your oral health, it is recommended to seek professional dental care for an accurate diagnosis and appropriate treatment.
What is the link between periodontal disease and cardiovascular disease?
Recent scientific research has shown a link between periodontal disease and cardiovascular disease, which refers to conditions that affect the heart and blood vessels, including heart attacks and strokes. While the exact mechanism by which periodontal disease contributes to cardiovascular disease is not fully understood, there are several theories.
One theory is that the bacteria that cause periodontal disease can enter the bloodstream through infected gum tissues and travel to other parts of the body, such as the heart. Once there, they can trigger an inflammatory response, leading to the development of arterial plaque and narrowing of the blood vessels, a condition known as atherosclerosis.
Another theory is that the inflammation caused by periodontal disease may increase the risk of blood clots, which can block blood flow to the heart or brain, leading to a heart attack or stroke.
Several studies have shown a correlation between periodontal disease and cardiovascular disease. For example, a study published in the American Journal of Cardiology found that people with severe periodontal disease were twice as likely to have heart disease than those without the condition.
What are periodontal disease treatment options?
The treatment options for periodontal disease depend on the stage and severity of the condition. The main goals of treatment are to control the infection, prevent further damage to the gums and supporting structures, and restore oral health. Here are some common treatment options:
Non-Surgical Treatments:
- Professional Dental Cleaning: This involves the removal of plaque and tartar (hardened plaque) from the teeth and below the gumline. It helps to reduce inflammation and control bacterial growth.
- Scaling and Root Planing: This procedure involves a deeper cleaning of the tooth roots and smoothing the rough surfaces to remove bacteria, toxins, and plaque. It helps in reducing pocket depths and promoting gum reattachment.
- Antibiotics: In some cases, antibiotics may be prescribed to control bacterial infection. They can be taken orally, applied directly to the gums, or placed into periodontal pockets.
Surgical Treatments:
- Flap Surgery: In this procedure, the gums are lifted to gain access to the tooth roots and underlying bone. The infected tissue is removed, and the bone may be reshaped. The gums are then repositioned to fit snugly around the teeth.
- Bone and Tissue Grafts: In advanced cases where there is significant bone and tissue loss, grafting procedures may be performed. This involves taking bone or tissue from another source (such as your own body or a synthetic material) and placing it in the affected area to promote regeneration of bone and tissue.
- Guided Tissue Regeneration: This technique involves placing a special barrier material between the gum tissue and bone to prevent gum tissue from growing into the bone space. This allows the bone and connective tissues to regenerate.
- Gum Grafts: If there is significant gum recession, gum grafts may be performed to cover exposed tooth roots. Gum tissue is taken from another area of the mouth or a donor source and placed over the recession site.
Specific treatment plans will vary depending on individual circumstances and the recommendations of your dentist or periodontist. After evaluating oral health, consider the extent of the disease, and develop a personalized treatment approach to address the needs.
How to prevent periodontal disease?
Prevention plays a crucial role in maintaining oral health and preventing periodontal disease. Here are some key steps you can take to help prevent the development or progression of gum disease:
Maintain Proper Oral Hygiene:
Brush your teeth at least twice a day using a fluoride toothpaste. Use a soft-bristled toothbrush and brush all surfaces of your teeth, including the gumline.
Floss daily to remove plaque and food particles from between your teeth and along the gumline. Consider using interdental brushes or water flossers if traditional flossing is challenging.
Consider using an antimicrobial mouthwash recommended by your dentist to help reduce bacteria in the mouth.
Visit Your Dentist Regularly:
Schedule regular dental check-ups and professional cleanings. Professional cleanings help remove plaque and tartar that cannot be eliminated through regular brushing and flossing.
Regular dental visits allow your dentist to monitor your oral health, detect early signs of gum disease, and provide appropriate treatment if necessary.
Adopt a Healthy Lifestyle:
Eat a balanced diet rich in fruits, vegetables, whole grains, and lean proteins. Limit sugary and acidic foods and drinks, as they can contribute to tooth decay and gum disease.
Avoid tobacco use in any form. Smoking and chewing tobacco are major risk factors for gum disease and can significantly impair your oral health.
Limit alcohol consumption, as excessive alcohol consumption can also increase the risk of gum disease.
Practice Stress Management:
High levels of stress can weaken the immune system and make you more susceptible to infections, including gum disease. Find healthy ways to manage stress, such as exercise, relaxation techniques, or engaging in activities you enjoy.
Manage Systemic Health Conditions:
Certain systemic conditions like diabetes can increase the risk of gum disease. Work with your healthcare provider to manage these conditions effectively, as it can positively impact your oral health as well.
Consider Genetic Factors:
Some individuals may have a genetic predisposition to gum disease. If you have a family history of periodontal problems, it is essential to be extra vigilant with your oral hygiene practices and maintain regular dental visits.
By following these preventive measures, you can significantly reduce your risk of developing periodontal disease and maintain optimal oral health.

What if I Have Symptoms?
If you have symptoms of periodontal disease, it is important to take prompt action and seek professional dental care. Here’s what you can do:
Schedule a Dental Appointment: Contact your dentist or periodontist as soon as possible to describe your symptoms and request an appointment. They will evaluate your oral health, conduct a thorough examination, and determine the appropriate course of action.
Describe Your Symptoms: During your dental appointment, provide a detailed description of your symptoms. Mention any signs of gum inflammation, bleeding, bad breath, changes in the appearance of your gums, or other concerns you may have. The more information you provide, the better your dentist can assess your condition.
Undergo a Comprehensive Examination: Your dentist will perform a comprehensive examination, which may include measuring pocket depths around your teeth, evaluating gum recession, assessing tooth mobility, and taking dental X-rays. These assessments help determine the extent and severity of your gum disease and guide the appropriate treatment plan.
Receive a Diagnosis and Treatment Plan: Based on the examination findings, your dentist will provide a diagnosis and recommend a treatment plan tailored to your specific needs. The treatment plan may include non-surgical treatments such as professional cleanings, scaling and root planing, or, in more advanced cases, surgical interventions.
Follow the Treatment Recommendations: It is crucial to follow your dentist’s recommendations for treatment. This may involve multiple visits for scaling and root planing or other procedures. Adhere to the prescribed oral hygiene practices and use any prescribed medications as instructed.
Maintain Regular Follow-up Visits: Periodontal disease requires ongoing management and monitoring. Attend follow-up visits as scheduled to allow your dentist to assess your progress, clean your teeth, and make any necessary adjustments to your treatment plan.
Early intervention is key in managing gum disease effectively. By seeking timely professional care, you can address the symptoms, prevent further progression of the disease, and work towards restoring your oral health.

Getting a Second Opinion
Getting a second opinion is a reasonable course of action if you have concerns about the diagnosis or treatment plan provided by your dentist. It can provide you with additional perspectives and help you make a well-informed decision about your oral health.
Research and Find Another Dental Professional: Look for another dentist or periodontist who specializes in periodontal disease. Seek recommendations from trusted sources such as family, friends, or healthcare professionals. You can also check online reviews or consult professional directories to find qualified dental professionals in your area.
Schedule an Appointment: Contact the dental professional you have chosen and explain that you would like a second opinion regarding your periodontal disease. Schedule an appointment at your convenience.
Share Relevant Information: Provide the new dental professional with your dental records, X-rays, and any other relevant information from your previous dentist. This will help them assess your condition and understand the previous diagnosis and treatment plan.
Discuss Your Concerns: During the appointment, discuss your symptoms, concerns, and any doubts you have about the previous diagnosis or treatment plan. Be open and transparent about your oral health history and any treatments you have received.
Evaluate the Second Opinion: After the examination and consultation, carefully consider the second opinion provided by the dental professional. Compare it with the initial diagnosis and treatment plan. Assess the similarities, differences, and the level of confidence you have in the recommendations.
Seeking a second opinion is your right as a patient, and it can help you gain clarity and confidence in your oral health treatment. It is essential to find a dental professional you trust and feel comfortable working with to ensure the best possible outcomes for your periodontal health.
FAQs
Conclusion
In conclusion, periodontal disease is not directly contagious but can be indirectly transmitted through the exchange of bacteria. Maintaining good oral hygiene, visiting dental professionals regularly, and adhering to preventive measures are essential for minimizing the risk of developing periodontal disease. By understanding the causes, risk factors, and transmission methods, individuals can take proactive steps to protect their oral health and prevent the spread of bacteria.

